In an era marked by technological leaps and bounds, the healthcare sector is no stranger to transformation. Yet, it is healthcare operations technology that holds the key to truly unlocking an era of unprecedented efficiency and patient care. Navigating the complexities of healthcare operations, however, is not without its challenges. From data accuracy to operational costs, healthcare providers and payers face a range of hurdles that can impede progress. We’ll dive into the pivotal role of healthcare operations technology and how it’s addressing these challenges, transforming the landscape of managed care, and leading the charge toward a more efficient and patient-focused future. Here are the topics we will explore in this article:
- The Gap in Healthcare Operations Technology
- Managed Care Data Accuracy Has Never Been More Crucial
- The Cost of Disconnected Point Solutions
- How to Overcome the Hurdles of Healthcare Operations Technology
The Gap in Healthcare Operations Technology
In the dynamic realm of healthcare, operations technology has grown over the years, paving the way for smarter patient care, and streamlined administrative processes. However, despite the massive strides made, there’s still a noticeable gap. Conventional systems often lack the level of automation and accuracy required in today’s digital landscape, leaving room for errors and inefficiencies. This gap underscores the urgent need for innovative solutions that blend human expertise with machine learning algorithms – a need that healthcare operations technology is perfectly suited to meet.
Managed Care Data Accuracy Has Never Been More Crucial
Data accuracy, the cornerstone of a flourishing healthcare ecosystem, takes on a profound significance in the realm of managed care. Managed care brings together providers and payers to collaboratively deliver the highest level of care to patients. This collaborative approach, however, requires precision in data to function smoothly.
The quality of patient care, efficient handling of reimbursement claims, and overall system effectiveness are all critically dependent on the precision and reliability of the underlying data. Hence, it is vital for providers and payers engaged in managed care programs like Medicaid and Medicare to adopt healthcare operations technology. This tech-forward approach ensures impeccable data accuracy, promotes adherence to compliance requirements, and significantly reduces the need for clarifications or unnecessary holds, thereby offering a more efficient and effective interaction.
The Cost of Disconnected Point Solutions
Technology has undeniably revolutionized the healthcare sector, transforming the way healthcare operations are managed. However, this evolution has also led to an influx of disconnected point solutions. Point solutions are specific software applications designed to tackle individual problems or fulfill specific functions within a broader system or business operation.
Many healthcare institutions continue to depend on numerous separate point solutions, that do not interact with one another, for a variety of operations, including patient data management, claims processing, compliance checks, and more. This fragmentation may seem efficient on the surface, with each solution tackling a unique challenge, but it often conceals a variety of issues underneath:
Higher Cost
Using multiple-point solutions can escalate operational costs significantly. Each solution comes with its own set of expenses, from initial acquisition and deployment costs to ongoing maintenance, upgrades, and staff training. These costs quickly add up, making the overall operations prohibitively expensive.
Inefficient
Managing multiple-point solutions can be highly inefficient. Different systems might not be designed to interact seamlessly with each other, which can create bottlenecks in information flow, hamper collaboration, slow down decision-making processes, and create more manual work. This fragmentation can limit the potential benefits of automation and digitization, leading to a frustratingly counterproductive situation.
Prone to Error
Using multiple solutions can increase the risk of data inconsistencies and inaccuracies. Each solution might interpret, process, and store data differently, leading to disparities that can negatively impact patient care, reimbursement claims, and compliance reporting. This also adds an extra layer of complexity when it comes to data security and privacy, with each solution posing its unique risks
By leveraging comprehensive healthcare operations technology, healthcare institutions can consolidate the functions originally used by separate point solutions, reduce errors and overhead, and streamline their operations in a more cohesive and efficient manner.
How to Overcome the Hurdles of Healthcare Operations Technology
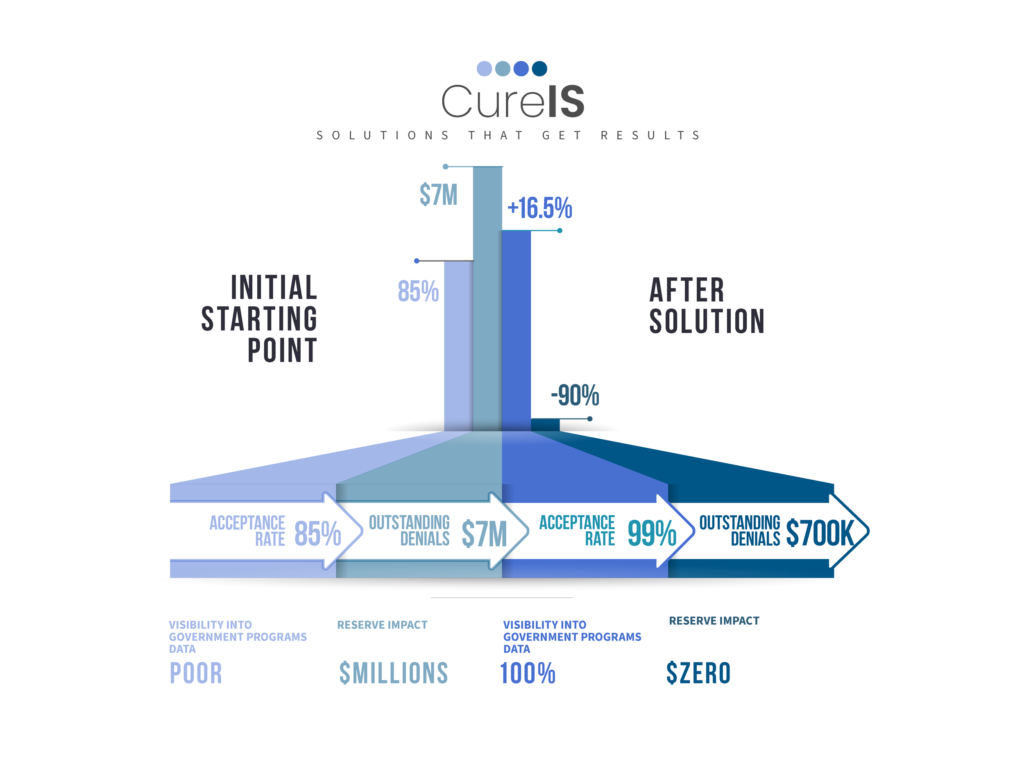
The road to embracing healthcare operations technology doesn’t come without its own set of challenges. However, the key to overcoming these hurdles is to work with a trusted partner that understands both sides of the healthcare equation. CureIS Healthcare provides managed services that optimize government programs, making managed care a focal point of their expertise. CureIS’ automated tools scrub data, ensuring it’s clean, compliant, and accurate, which decreases risk, expedites reimbursement times, and guarantees end-to-end accountability.
The CureIS difference lies in its ability to transform healthcare operations. Replacing manual data entry with automated processes powered by the latest in claims administration and compliance knowledge. The result? Minimal errors, faster turnaround times, and improved strategies – all of which are fundamental in enhancing the quality of patient care and driving operational excellence in the healthcare industry.
Embracing healthcare operations technology, therefore, is no longer optional but vital for any healthcare institution aiming to improve patient care and operational efficiency. By bridging the existing gap and putting the focus back on accurate, efficient, and automated processes, providers and payers can collaboratively redefine the future of managed care.
At CureIS, we offer automated, optimized solutions for government healthcare programs. We’re dedicated to helping you focus on what truly matters: exceptional patient care. Get in touch with the CureIS team today, and let’s revolutionize your healthcare operations.